How Lifestyle Changes Can Support Sleep Apnea Treatment
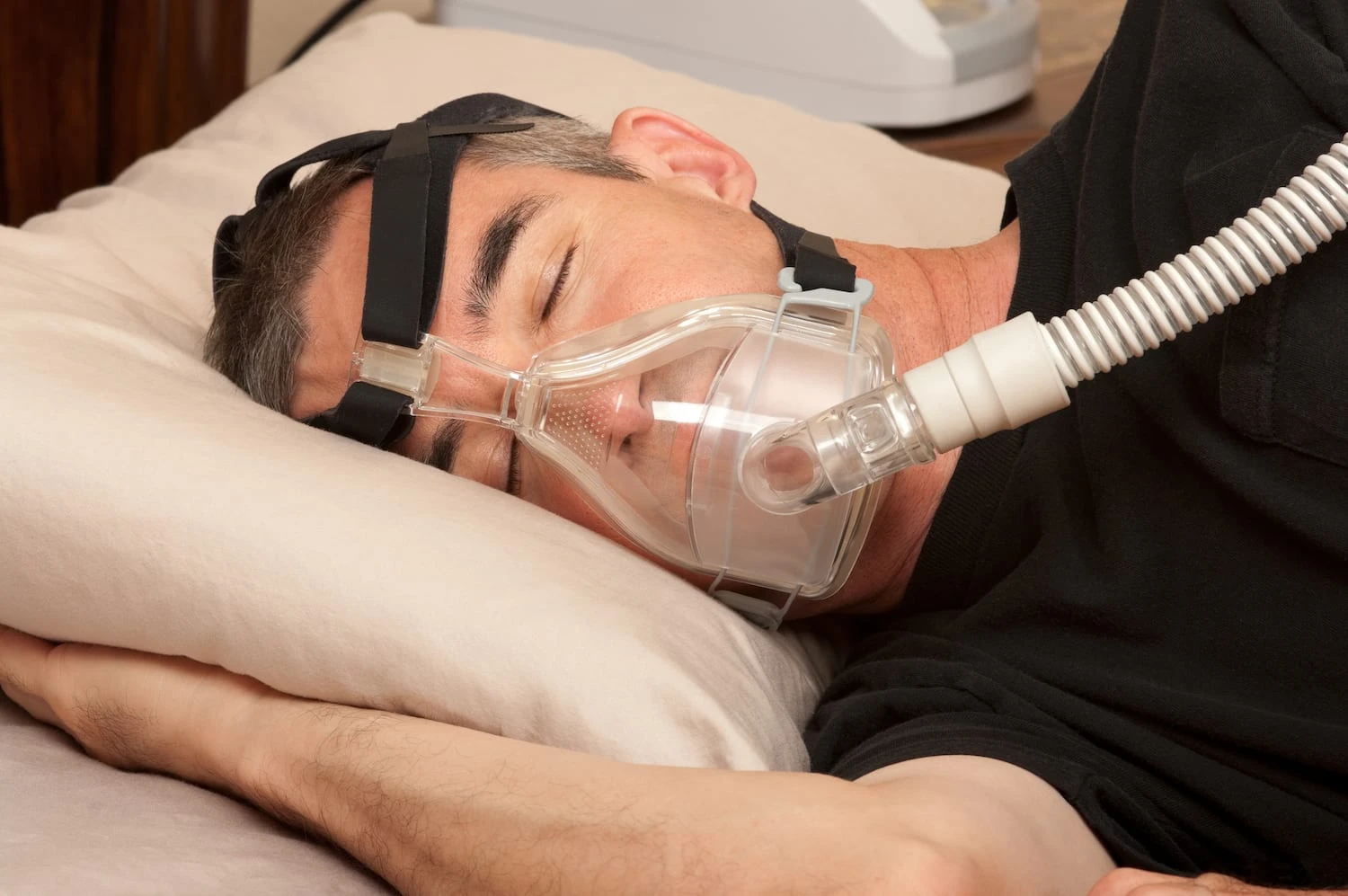
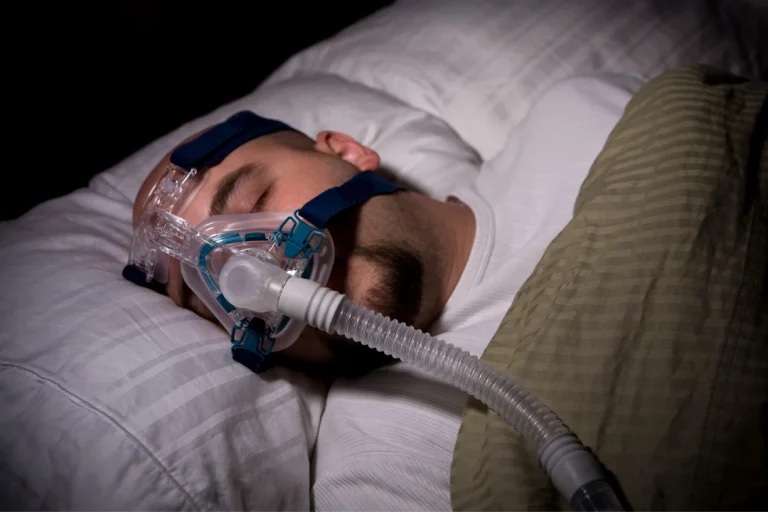
The most effective way to support sleep apnea treatment involves a combination of weight management, positional therapy, and avoidance of central nervous system depressants like alcohol. Reducing excess body fat, particularly around the neck, decreases physical pressure on the airway, while sleeping on one’s side prevents the tongue and soft palate from collapsing backward during sleep. Vector Sleep Diagnostic Center has analyzed thousands of sleep studies and consistently finds that patients who integrate these specific behavioral modifications with prescribed medical therapies experience significantly better outcomes. This guide will explain exactly how these changes work physiologically and how to implement them in a daily routine.
The Impact of Weight on Airway Patency
Excess body weight remains the single most significant modifiable risk factor for obstructive sleep apnea. Fat deposits around the upper airway can narrow the breathing passage, while abdominal fat can compress the chest wall, reducing lung volume. Research shows that even a modest weight reduction of 10 to 15 percent of body weight can lead to a substantial decrease in apnea severity.
The relationship between weight and sleep is cyclical. Poor sleep disrupts hormones that regulate hunger, specifically ghrelin and leptin, leading to increased cravings for high-calorie foods. By breaking this cycle through dietary adjustments, patients can improve both their sleep quality and metabolic health. Vector Sleep Diagnostic Center frequently observes that patients who commit to a sustainable, rather than drastic, weight loss plan maintain their results longer.
Positional Therapy and Gravity
Gravity plays a major role in the collapse of the airway during sleep. For many individuals, apnea events occur primarily when sleeping on their backs, known as the supine position. In this posture, the tongue and soft tissues naturally fall backward due to gravity, obstructing airflow. Shifting to a side-sleeping position often keeps the airway open enough to prevent obstructions.
Comparing Sleep Positions
The table below outlines how different sleeping positions affect airway mechanics for those with sleep apnea.
| Sleep Position | Airway Stability | Risk Level | Mechanical Effect |
|---|---|---|---|
| Back (Supine) | Low | High | Gravity pulls the tongue and soft palate backward, narrowing the airway. |
| Side (Lateral) | High | Low | Tissues fall to the side, keeping the airway channel relatively clear. |
| Stomach (Prone) | Medium | Medium | Keeps the airway open but can cause neck strain and restricted breathing. |
Transitioning to side sleeping can be difficult for those accustomed to sleeping on their backs. Using a body pillow or placing a tennis ball in a pocket sewn onto the back of a shirt can prevent rolling over during the night.
The Role of Diet and Exercise
While weight loss is a primary goal, the specific types of food consumed also affect muscle tone and inflammation. Diets high in processed sugars and saturated fats contribute to systemic inflammation, which can cause swelling in the tissues lining the throat. Anti-inflammatory diets, rich in vegetables, fruits, and lean proteins, help maintain the structural integrity of the airway muscles.
Exercise provides benefits beyond calorie burning. Regular physical activity improves sleep quality and respiratory muscle strength. Aerobic exercises, such as brisk walking or swimming, increase overall lung capacity and oxygen efficiency.
Myofunctional Therapy
Specific exercises targeting the muscles of the mouth and throat can strengthen the airway. Known as oropharyngeal or myofunctional therapy, these exercises involve actions like tongue presses and soft palate lifting. A study published by the National Institutes of Health indicates that these exercises can reduce the severity of obstructive sleep apnea by approximately 50 percent in some patients.
Managing Substances and Environment
What enters the body before bed has an immediate effect on airway stability. Alcohol acts as a muscle relaxant, causing the throat muscles to collapse more easily than usual. It also affects the brain’s ability to arouse from sleep when breathing stops, leading to longer and more dangerous pauses in breathing. Avoiding alcohol for at least three to four hours before bed is a standard recommendation.
Regional Considerations
Environmental factors differ based on geography and climate. In regions with high humidity or for individuals living in dry climates, maintaining optimal humidity in the bedroom is essential. Dry air can irritate mucous membranes, causing swelling that narrows the airway. Conversely, excessive humidity can encourage mold growth, which triggers allergies and congestion. Using a humidifier with a built-in hygrometer ensures the room stays within the optimal 30 to 50 percent humidity range.
Smoking cessation is equally important. Smoking causes upper airway inflammation and fluid retention in the throat. The nicotine withdrawal cycle can also disrupt sleep architecture.

Market Data and Prevalence
Understanding the scope of sleep apnea highlights why lifestyle intervention is necessary. According to the Sleep Foundation, approximately 30 million adults in the United States have obstructive sleep apnea, though a vast majority remain undiagnosed. The prevalence of this condition has risen steadily over the last two decades, mirroring the global rise in obesity rates.
Data from Mayo Clinic also suggests that the economic burden of undiagnosed sleep apnea in the United States is substantial, taking a massive toll each year through lost productivity, motor vehicle accidents, and workplace errors. These statistics underscore the importance of proactive management through lifestyle changes.
Things to Consider Before Making a Decision
Before overhauling a daily routine, patients should evaluate several factors to ensure success.
- Severity of Apnea: Lifestyle changes work best for mild to moderate cases. Severe cases typically require immediate medical intervention like CPAP therapy alongside lifestyle changes.
- Comorbid Conditions: Hypertension, heart disease, and diabetes require careful coordination between sleep specialists and primary care physicians.
- Personal Readiness: drastic changes often fail. Small, incremental adjustments are more sustainable and effective in the long run.
- Sleep Environment: Evaluating the bedroom for light, noise, and temperature issues is a prerequisite for good sleep hygiene.
Common Questions
Many patients wonder if dietary changes alone can cure the condition. While significant weight loss can lead to remission in some, it rarely “cures” the underlying anatomical predisposition permanently. Apnea often returns if weight is regained. Another common concern involves the permanence of positional therapy. For back sleepers, changing position is a lifelong adjustment, not a temporary fix.
Bonus Tips
- Elevate the Head: Raising the head of the bed by a few inches using risers or a wedge pillow can help prevent the tongue from falling backward. This uses gravity to assist the airway.
- Consistent Schedule: Going to bed and waking up at the same time every day regulates the circadian rhythm, which can stabilize breathing patterns during sleep.
- Hydration: Drinking plenty of water throughout the day keeps the throat mucous membranes lubricated, reducing the likelihood of tissue sticking together or vibrating.
Conclusion
Supporting sleep apnea treatment requires a multifaceted approach focused on reducing anatomical obstructions and improving overall health. Weight management, positional therapy, and the elimination of muscle relaxants like alcohol are the pillars of this strategy. While these changes require discipline, they offer benefits that extend far beyond the bedroom, improving cardiovascular health, mood, and longevity. Readers should assess their current habits, consult with a specialist, and implement these changes gradually to ensure lasting improvement in their condition.
Contact Vector Sleep Diagnostic Center
To accurately determine the severity of your condition and track the progress of your lifestyle changes, a professional evaluation is essential. Vector Sleep Diagnostic Center provides comprehensive sleep studies that offer the data needed to tailor your treatment plan effectively.
To schedule a consultation or sleep study, reach out via email at vectorsleep@gmail.com or call +1 718-830-2800. Our medical team is available to answer questions and guide patients through the process of achieving better sleep.
Frequently Asked Questions
Does sleeping position really matter that much?
Yes, for positional obstructive sleep apnea, sleeping on the back can double or triple the number of breathing events compared to side sleeping.
Can exercise cure sleep apnea without weight loss?
While weight loss is the primary mechanism, aerobic exercise improves sleep quality and respiratory muscle function independent of weight changes, potentially reducing severity.
Is it necessary to give up caffeine completely?
Caffeine does not need to be eliminated entirely, but avoiding it at least six hours before bedtime helps prevent sleep fragmentation and insomnia.
How long does it take for lifestyle changes to show results?
Most patients begin to notice improvements in energy levels within two weeks, but measurable changes in sleep study data, such as the Apnea-Hypopnea Index, may take three to six months of consistent effort.
Do nasal strips help with sleep apnea?
Nasal strips can improve airflow through the nose if congestion is an issue, but they generally do not prevent the collapse of the soft palate at the back of the throat, which is the main cause of obstructive sleep apnea.
Sources
- National Institutes of Health – A peer-reviewed study detailing the efficacy of oropharyngeal exercises in reducing obstructive sleep apnea severity.
- Sleep Foundation – Comprehensive statistics regarding the prevalence, economic costs, and risk factors associated with sleep apnea.
- Mayo Clinic – Detailed medical information on self-care strategies and lifestyle adjustments for managing sleep apnea.