From Snoring to Sleep Apnea: How a Sleep Study Helps Diagnose Issues
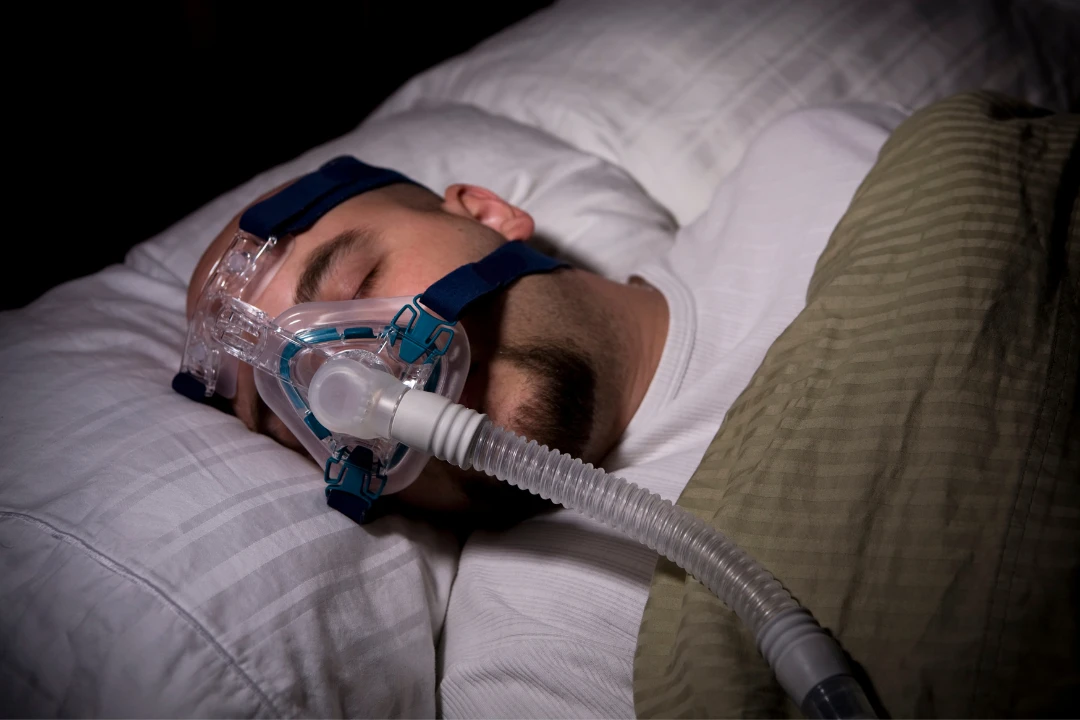
A sleep study, known as polysomnography, provides the definitive answer to distinguish between harmless snoring and potentially life-threatening sleep apnea by monitoring your breathing patterns, brain activity, oxygen levels, and body movements throughout the night. While loud snoring often serves as the first warning sign, only a comprehensive sleep study can accurately measure how often your breathing stops, the severity of oxygen deprivation, and whether your sleep architecture is being disrupted. This diagnostic tool gives sleep specialists the specific data needed to determine if you have sleep apnea and how severe it might be.
This guide breaks down everything you need to know about sleep studies, from what happens during the test to how results inform treatment decisions. Vector Sleep Diagnostic Center has conducted thousands of these studies, helping people finally understand why they feel exhausted despite spending hours in bed.
Understanding the Difference Between Snoring and Sleep Apnea
Snoring and sleep apnea might sound similar, but they represent vastly different medical conditions. Snoring occurs when air flows past relaxed tissues in your throat, causing them to vibrate as you breathe. It’s annoying for bed partners but typically harmless. Sleep apnea, however, involves repeated episodes where your breathing completely stops for 10 seconds or longer, sometimes hundreds of times per night.
The key difference lies in oxygen levels. With regular snoring, your oxygen saturation remains normal throughout the night. In sleep apnea cases, these breathing pauses cause oxygen levels to drop repeatedly, forcing your brain to partially awaken you to resume breathing. This cycle prevents the deep, restorative sleep your body needs.
Most people with sleep apnea don’t realize they’re stopping breathing. The fragmented sleep leads to daytime sleepiness, morning headaches, difficulty concentrating, and increased risks of serious health conditions like heart disease, stroke, and diabetes. According to research published in the American Journal of Respiratory and Critical Care Medicine, approximately 25% of adults have sleep-disordered breathing, with many cases going undiagnosed.
What Exactly Happens During a Sleep Study
A sleep study sounds intimidating, but it’s a straightforward and painless procedure. You’ll arrive at a sleep center in the evening, get changed into comfortable sleepwear, and have sensors applied to various parts of your body. These sensors monitor brain waves, eye movements, heart rate, breathing patterns, blood oxygen levels, and muscle activity.
The setup typically takes about 30-45 minutes. The electrodes are small and connected with thin wires that allow you to move freely. Once everything is attached, you’ll sleep in a private room designed to feel like a comfortable hotel room. A technician monitors your sleep from a nearby control room but won’t disturb you unless absolutely necessary.
The goal is to capture a typical night’s sleep. Don’t worry if you think you won’t sleep well—the test only needs a few hours of sleep data to be effective. Even if you’re nervous, the technicians are trained to help you feel comfortable and adjust the equipment if needed.
Bonus Tip: Avoid caffeine and alcohol after noon on the day of your study. Both substances can significantly disrupt sleep patterns and affect the accuracy of your results.
Types of Sleep Studies and What They Measure
Not all sleep studies are the same. The type of test you’ll undergo depends on your specific symptoms and what your doctor needs to diagnose. The most common is an in-lab polysomnography, which provides the most comprehensive data about your sleep.
However, home sleep apnea tests have become increasingly popular. These simplified devices measure breathing effort, airflow, and blood oxygen levels but don’t capture brain activity or muscle movements. According to data from the American Academy of Sleep Medicine, home sleep tests cost significantly less than in-lab studies and can effectively diagnose moderate to severe sleep apnea in many patients.
Here’s how the different approaches compare:
| Study Type | What It Measures | Best For |
|---|---|---|
| In-lab polysomnography | Brain waves, eye movements, heart rate, breathing, oxygen, muscle activity | Complex cases, other sleep disorders, surgery planning |
| Home sleep test | Breathing effort, airflow, oxygen levels | Straightforward apnea cases, high pre-test probability |
| Multiple sleep latency test | How quickly you fall asleep during daytime naps | Diagnosing narcolepsy, excessive daytime sleepiness |
| Maintenance of wakefulness test | Your ability to stay awake during quiet activities | Assessing treatment effectiveness, safety-critical jobs |

Interpreting Sleep Study Results
The most important metric from a sleep study is the Apnea-Hypopnea Index (AHI), which measures how many breathing disruptions occur per hour. This number determines whether you have sleep apnea and how severe it is.
An AHI below 5 is considered normal. Between 5-15 indicates mild sleep apnea, 15-30 is moderate, and above 30 is severe. But the numbers only tell part of the story. Sleep specialists also look at oxygen desaturation levels, how often your brain wakes up, and how much time you spend in each sleep stage.
For example, someone might have a moderate AHI but experience severe oxygen drops, requiring more aggressive treatment. Another person might have frequent awakenings with only mild breathing issues, suggesting different interventions. The comprehensive data from a sleep study allows for personalized treatment plans rather than one-size-fits-all approaches.
Bonus Tip: Ask for a copy of your sleep study report and have your doctor explain what each section means. Understanding your specific patterns helps you participate more actively in your treatment decisions.
Things to Consider Before Making a Decision
Before undergoing a sleep study, several practical considerations can help ensure you get the most accurate results and comfortable experience. Insurance coverage varies widely between in-lab and home studies, so check your benefits beforehand. Some plans require you to try a home test first before approving an in-lab study.
Your sleep habits matter too. If you typically sleep poorly in unfamiliar environments, discuss this with the sleep center staff. They might suggest bringing your own pillow, avoiding daytime naps before the study, or practicing relaxation techniques. Sleep centers understand these concerns and have strategies to help you sleep naturally.
The National Sleep Foundation reports that untreated sleep apnea increases the risk of motor vehicle accidents by up to six times due to daytime sleepiness. This context helps explain why doctors take these symptoms seriously and recommend proper testing rather than ignoring warning signs.
Bonus Tip: Keep a sleep diary for two weeks before your study. Note when you go to bed, how long it takes to fall asleep, nighttime awakenings, and how rested you feel each morning. This information complements the objective data from your study.
Next Steps for Better Sleep
Understanding whether your snoring is merely annoying or a sign of serious sleep apnea starts with proper diagnostic testing. Sleep studies provide the objective data needed to distinguish between these conditions and guide appropriate treatment. The information gained can literally save your life by reducing risks of heart disease, stroke, and accidents related to daytime sleepiness.
If you’ve been told you snore loudly, gasp for air during sleep, or feel exhausted despite adequate sleep time, consider discussing a sleep study with your healthcare provider. The path to restful nights and energized days begins with accurate diagnosis and personalized treatment based on your specific sleep patterns.
Take Control of Your Sleep Health Today
Vector Sleep Diagnostic Center offers comprehensive sleep studies to help identify and treat sleep disorders effectively. Don’t let another restless night affect your health, relationships, and quality of life. Contact us at vectorsleep@gmail.com or call +1 718-830-2800 to schedule a consultation. Taking this step could transform your days and protect your long-term health.
FAQS
Can a sleep study detect other sleep disorders besides apnea?
Yes, polysomnography can identify narcolepsy, periodic limb movement disorder, REM sleep behavior disorder, and various parasomnias like sleepwalking. The comprehensive monitoring captures abnormalities across multiple body systems.
How long does it take to get results?
Most sleep centers provide results within 1-2 weeks. The data needs technical scoring by a sleep technologist and interpretation by a board-certified sleep medicine physician before a formal report is generated.
What if I need to use the bathroom during the night?
Sleep technicians provide a call button, and they can quickly disconnect you from monitoring equipment when needed. This process typically takes only a minute, so you can return to sleep with minimal disruption.
Will my medication affect the sleep study results?
Certain medications can influence sleep architecture and breathing patterns. Always provide a complete list of medications, supplements, and dosages before your study. Your doctor may advise continuing or temporarily stopping specific medications.
Is sleep apnea always treated with a CPAP machine?
While CPAP (continuous positive airway pressure) is the gold standard treatment, alternatives exist for mild to moderate cases. Options include oral appliances from dentists, positional therapy devices, weight management programs, and in some cases, surgical procedures.
Sources
- American Journal of Respiratory and Critical Care Medicine – Peer-reviewed medical journal publishing research on respiratory and critical care medicine
- American Academy of Sleep Medicine – Professional organization setting standards and guidelines for sleep medicine practice


